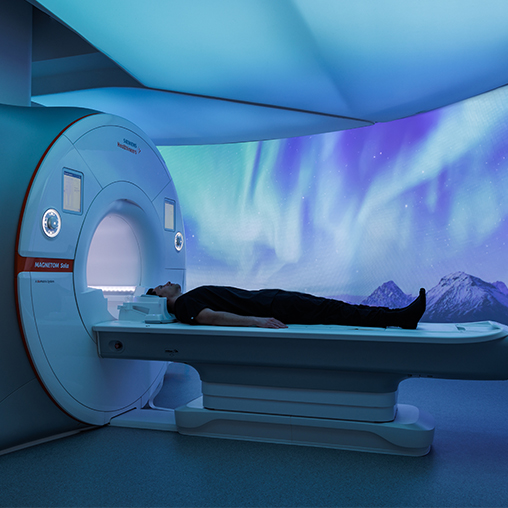
Realizing the Value of Artificial Intelligence When Planning Tomorrow’s Healthcare Facilities
The true value of AI lies not just in its ability to revolutionize devices and treatments but in its power to drive ROI through smarter, more adaptable healthcare environments.
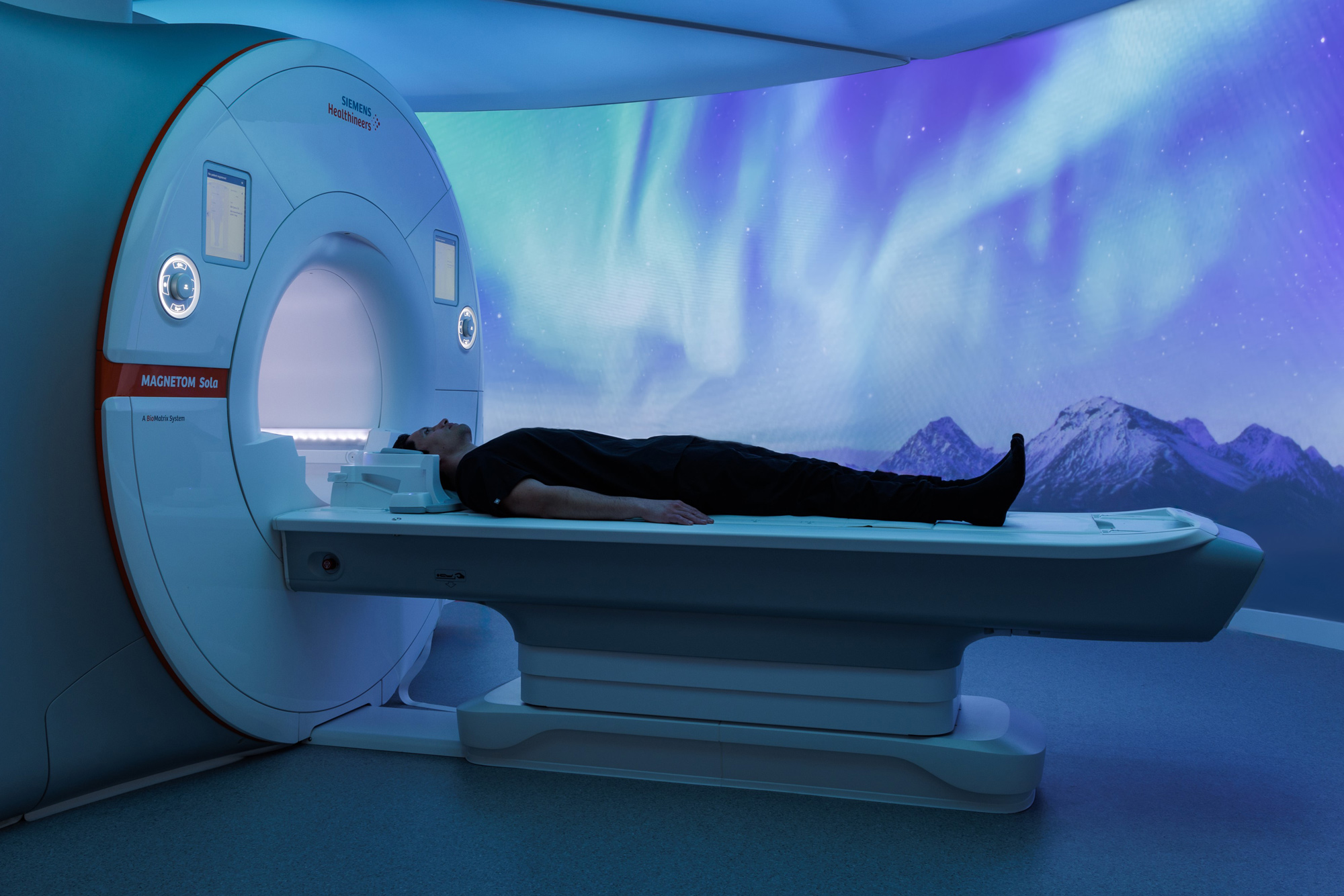
Artificial intelligence is revolutionizing healthcare, not only by enhancing efficiency and improving patient experiences but also by redefining the value of investing in adaptable, future-proof infrastructure. As medical technologies evolve at a pace far exceeding the lifespans of the buildings designed to house them, it is crucial for the architecture and construction industry to rise to the challenge of adaptability.
AI offers a transformative opportunity to bridge this gap, enabling smarter design processes that align with the dynamic nature of healthcare.
In recent years, investment in generative AI has skyrocketed, reshaping industries and accelerating innovation. Yet, the buildings that house these innovations often lag in adaptability. This disparity raises a critical question: how can we design healthcare environments that keep pace with technological change and maximize their long-term value? The true value of AI lies not just in its ability to revolutionize devices and treatments but in its power to drive return on investment through smarter, more adaptable healthcare environments.
The Gap Between Innovation and Infrastructure
While investment in construction technology has doubled over the past decade, according to McKinsey & Company, the pace of healthcare innovation still far outstrips advancements in the built environment. Medical devices and AI-enabled systems are evolving faster than the facilities designed to accommodate them. Buildings, with lifespans often exceeding 50 years, must be planned with flexibility in mind to adapt to these shorter technology cycles.
For designers, this gap represents an opportunity. Understanding the trajectory of healthcare innovation can help clients future-proof their investments, ensuring facilities remain relevant and functional for decades to come. This involves rethinking traditional approaches to design and embracing modular, adaptable layouts that can evolve alongside advancements in medical technology.
Defining Value in Healthcare Design
Value in healthcare is multifaceted — encompassing efficiency, patient satisfaction, and long-term functionality. Architects play a pivotal role in shaping these environments, ensuring they not only meet current demands but also anticipate future needs. Now is the time to invest in adaptable, future-proof designs. Constructing with the future of AI in mind has the following main benefits:
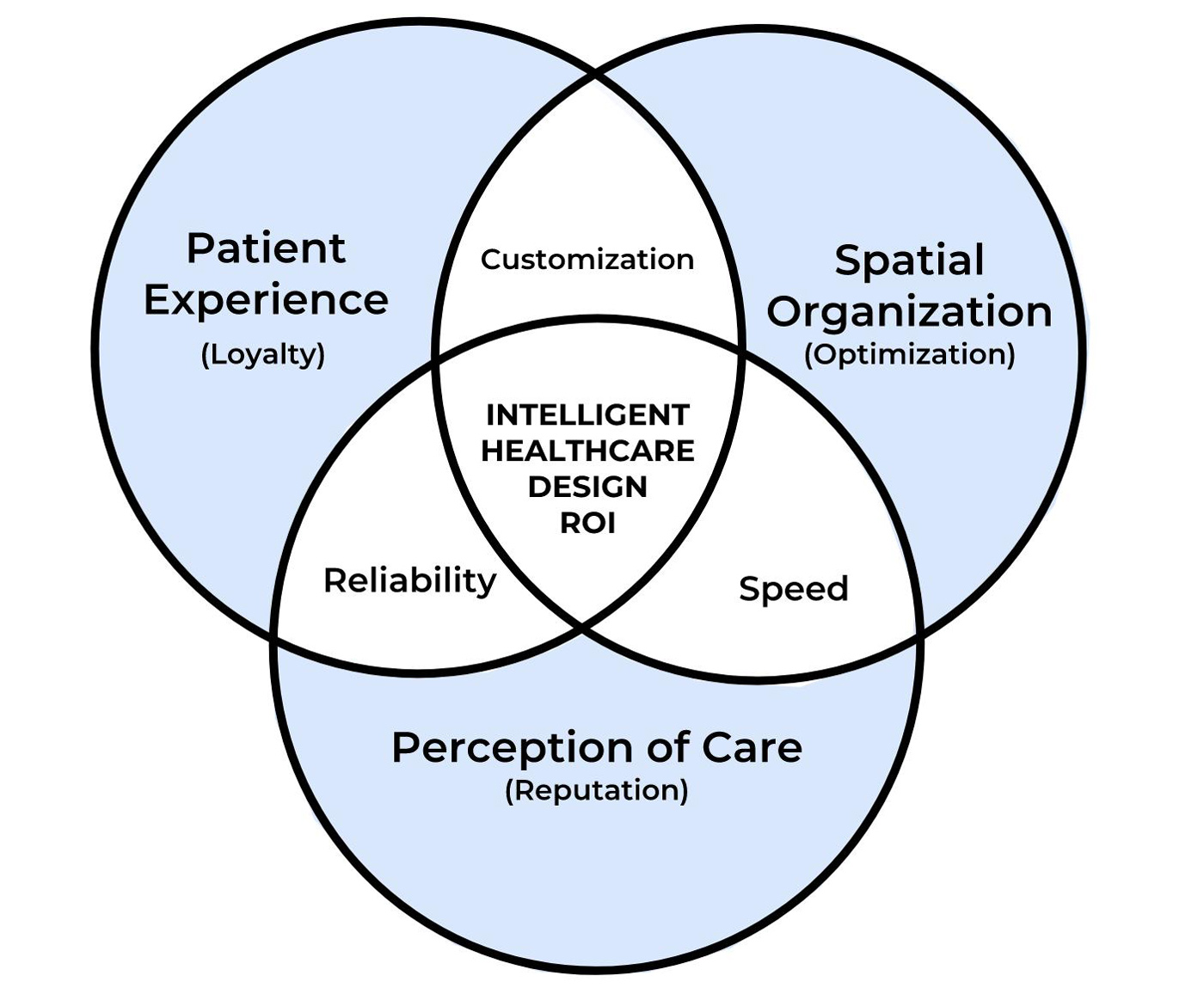
- Optimization: Spatial organization is the key factor in travel distances, operational efficiencies, and ultimately doctor-patient care time. AI can analyze patient volume, forecast admissions, and determine staffing needs, enabling more precise resource allocation and streamlined operations. For example, predictive tools can estimate patient length of stay, informing decisions about room counts and department layouts.
- Reputation: Perception of care is increasingly influenced by factors beyond direct medical treatment, including the look and feel of the environment, waiting time, cost of medical service, or easy access to the facility. AI can help improve time management and reduce patient wait times, enhancing the overall experience and building trust.
- Loyalty: A positive patient experience fosters loyalty. In an era of private medical services, patients have a choice of where to receive healthcare. AI-driven insights into behavior and preferences can help designers create environments that prioritize comfort and accessibility, ensuring patients choose to return.
By integrating AI into the design process, architects can support a greater ROI through predictive insights to optimize spatial layouts, improve resource allocation, and enhance patient experiences. This collaboration between AI and design positions architects as strategic partners in healthcare innovation, driving environments that are resilient, adaptable, and aligned with the accelerating pace of medical advancement.
Leveraging AI for Intelligent Healthcare Design
Architects can use AI to revolutionize healthcare space planning by combining deep insights from data with design strategies that prioritize efficiency, adaptability, and care outcomes. This includes:
Spatial Organization: By leveraging AI to streamline operations and enhance environmental aesthetics, architects can design spaces that build trust, reinforce institutional reputation, and improve the overall patient experience. In addition, AI tools can analyze patient volumes and predict resource needs, ensuring facilities are appropriately scaled. For instance, AI can forecast patient admissions and staff requirements, enabling more accurate program KPU requirements, which ultimately better size the project.
Infection control & inventory management: AI-driven safety strategies, such as live germ spread analysis and smart HVAC systems, optimize air quality and minimize contamination risks. These tools track behavior and proximity to mitigate infection risks, creating safer environments.
AI can also streamline supply chain operations, predicting just-in-time delivery needs and managing surge inventory capacity. This reduces redundancy and maximizes back-of-house efficiency.
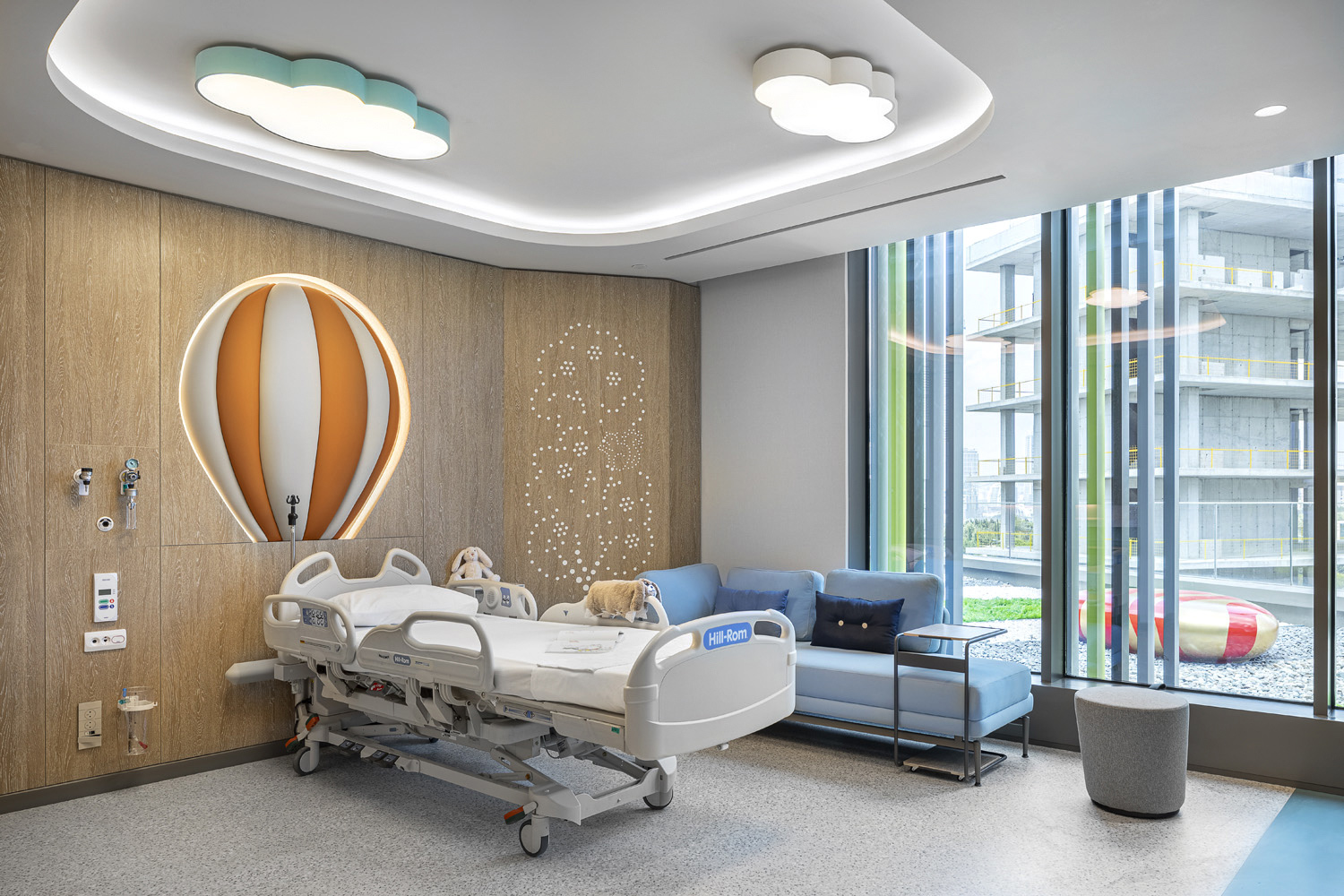
Perception of Care: The architect’s ability to craft spaces that enhance patient experience is amplified through AI, which provides real-time insights into behavior and preferences. By integrating personalized environmental controls and adaptive design strategies, architects can create spaces that comfort, engage, and empower patients. AI can optimize scheduling and track patient throughput, reducing wait times, improving caregiver/patient interaction, and positively influencing the perception of care. These enhancements directly impact patient satisfaction, as reflected in post-visit surveys. Data analytics with AI also can provide actionable insights into patient flow and staff utilization, enabling facilities to recalibrate operations for maximum efficiency.
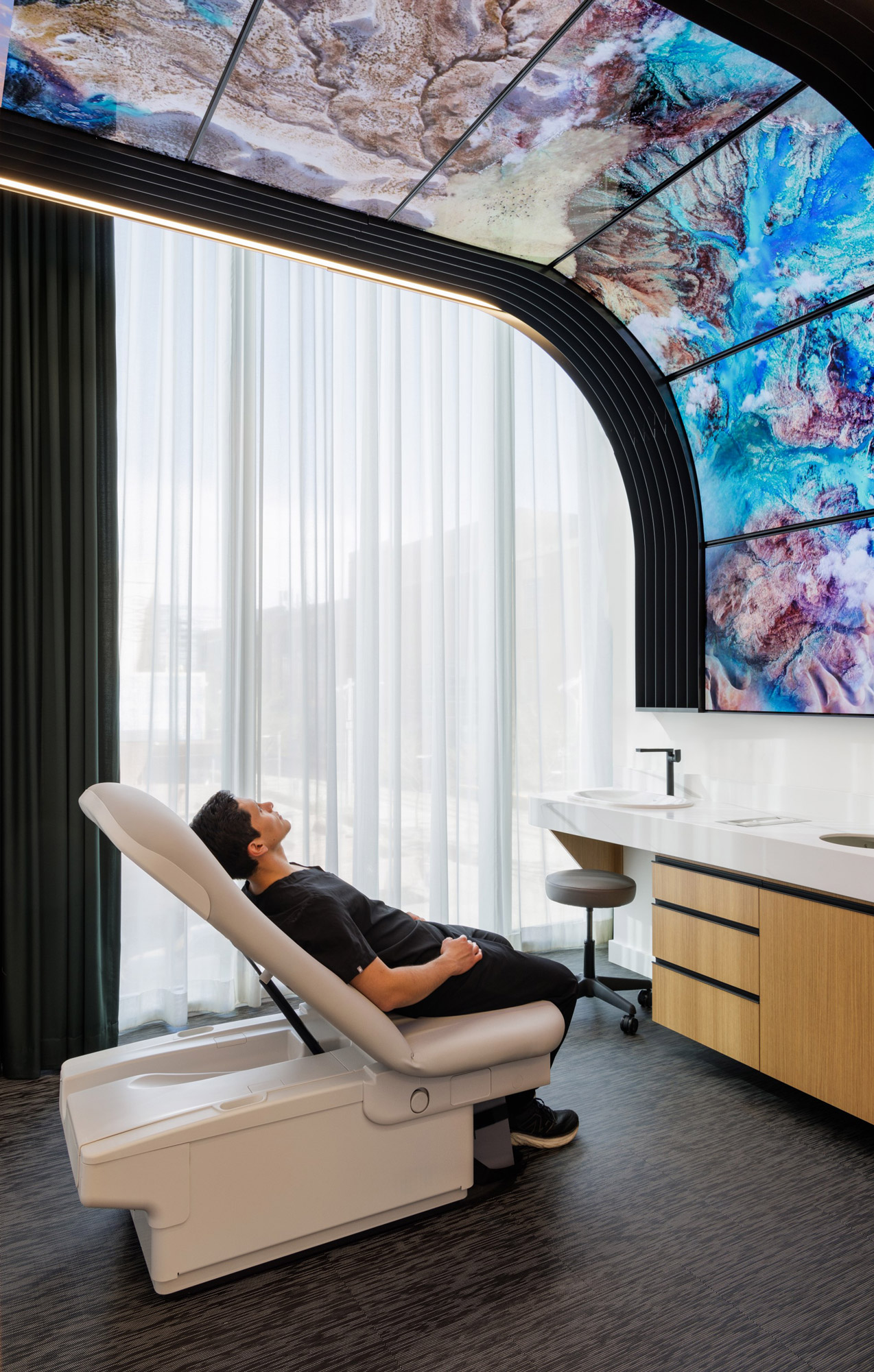

Patient Experience: AI enhances the patient experience by creating environments tailored to individual needs. This may be in the form of a behavioral pattern analysis to influence design decisions.
Technologies like virtual reality and eye-tracking help identify sightlines and functional areas within a space, optimizing layouts for usability and comfort.
AI-driven systems allow for the adjustment of environmental factors like lighting, sound, and graphics in real-time based on patient vitals and stress levels. This personalization improves comfort and reduces anxiety, particularly in scenarios like MRI scans. Chatbot-enabled systems allow patients to adjust their surroundings, from lighting to bed positions, enhancing their sense of control and comfort.
Future-Proofing Healthcare Facilities
The rapid integration of AI into healthcare underscores the importance of designing facilities that can adapt to future changes. Modular layouts and flexible infrastructure are essential for accommodating evolving technologies and workflows. Designers must anticipate shifts in healthcare delivery and create environments that support innovation without requiring extensive renovations.
The value of AI in healthcare extends far beyond the technology itself. By strategically leveraging AI, architects bridge the gap between healthcare innovation and construction, delivering environments that maximize ROI for patients, providers, and the industry as a whole. Their expertise is the foundation for navigating the complexities of this rapidly evolving landscape and ensuring that healthcare spaces are both innovative and enduring.
For media inquiries, email .